Decent/obvious report…
http://www.pwc.com/us/en/health-industries/healthcare-new-entrants/business-implications.jhtml
PDF: pwc-hri-new-entrants
Decent/obvious report…
http://www.pwc.com/us/en/health-industries/healthcare-new-entrants/business-implications.jhtml
PDF: pwc-hri-new-entrants
http://www.abc.net.au/radionational/programs/saturdayextra/japan27s-aging-population/5397864
A quarter of Japanese people are now aged over 65, with predictions that nearly half the population will reach that age by the end of the century.
In Japan people don’t just live longer, they work longer, stay healthier and approach old age in some interesting and innovative ways.
One policy initiative is old age day care which is well used and well organised in Japan.
Mammography = bad, according to the Swiss…
http://www.nejm.org/doi/full/10.1056/NEJMp1401875?query=TOC
Perspective
April 16, 2014DOI: 10.1056/NEJMp1401875
Article
In January 2013, the Swiss Medical Board, an independent health technology assessment initiative under the auspices of the Conference of Health Ministers of the Swiss Cantons, the Swiss Medical Association, and the Swiss Academy of Medical Sciences, was mandated to prepare a review of mammography screening. The two of us, a medical ethicist and a clinical epidemiologist, were members of the expert panel that appraised the evidence and its implications. The other members were a clinical pharmacologist, an oncologic surgeon, a nurse scientist, a lawyer, and a health economist. As we embarked on the project, we were aware of the controversies that have surrounded mammography screening for the past 10 to 15 years. When we reviewed the available evidence and contemplated its implications in detail, however, we became increasingly concerned.
First, we noticed that the ongoing debate was based on a series of reanalyses of the same, predominantly outdated trials. The first trial started more than 50 years ago in New York City and the last trial in 1991 in the United Kingdom.1 None of these trials were initiated in the era of modern breast-cancer treatment, which has dramatically improved the prognosis of women with breast cancer. Could the modest benefit of mammography screening in terms of breast-cancer mortality that was shown in trials initiated between 1963 and 1991 still be detected in a trial conducted today?
Second, we were struck by how nonobvious it was that the benefits of mammography screening outweighed the harms. The relative risk reduction of approximately 20% in breast-cancer mortality associated with mammography that is currently described by most expert panels2 came at the price of a considerable diagnostic cascade, with repeat mammography, subsequent biopsies, and overdiagnosis of breast cancers — cancers that would never have become clinically apparent. The recently published extended follow-up of the Canadian National Breast Screening Study is likely to provide reliable estimates of the extent of overdiagnosis. After 25 years of follow-up, it found that 106 of 484 screen-detected cancers (21.9%) were overdiagnosed.3 This means that 106 of the 44,925 healthy women in the screening group were diagnosed with and treated for breast cancer unnecessarily, which resulted in needless surgical interventions, radiotherapy, chemotherapy, or some combination of these therapies. In addition, a Cochrane review of 10 trials involving more than 600,000 women showed there was no evidence suggesting an effect of mammography screening on overall mortality.1 In the best case, the small reduction in breast-cancer deaths was attenuated by deaths from other causes. In the worst case, the reduction was canceled out by deaths caused by coexisting conditions or by the harms of screening and associated overtreatment. Did the available evidence, taken together, indicate that mammography screening indeed benefits women?
Third, we were disconcerted by the pronounced discrepancy between women’s perceptions of the benefits of mammography screening and the benefits to be expected in reality. The figure U.S. Women’s Perceptions of the Effects of Mammography Screening on Breast-Cancer Mortality as Compared with the Actual Effects. shows the numbers of 50-year-old women in the United States expected to be alive, to die from breast cancer, or to die from other causes if they are invited to undergo regular mammography every 2 years over a 10-year period, as compared with women who do not undergo mammography. The numbers in Panel A are derived from a survey about U.S. women’s perceptions,4 in which 717 of 1003 women (71.5%) said they believed that mammography reduced the risk of breast-cancer deaths by at least half, and 723 women (72.1%) thought that at least 80 deaths would be prevented per 1000 women who were invited for screening. The numbers in Panel B reflect the most likely scenarios according to available trials1-3: a relative risk reduction of 20% and prevention of 1 breast-cancer death. The data for Switzerland, reported in the same study, show similarly overly optimistic expectations. How can women make an informed decision if they overestimate the benefit of mammography so grossly?
U.S. Women’s Perceptions of the Effects of Mammography Screening on Breast-Cancer Mortality as Compared with the Actual Effects. shows the numbers of 50-year-old women in the United States expected to be alive, to die from breast cancer, or to die from other causes if they are invited to undergo regular mammography every 2 years over a 10-year period, as compared with women who do not undergo mammography. The numbers in Panel A are derived from a survey about U.S. women’s perceptions,4 in which 717 of 1003 women (71.5%) said they believed that mammography reduced the risk of breast-cancer deaths by at least half, and 723 women (72.1%) thought that at least 80 deaths would be prevented per 1000 women who were invited for screening. The numbers in Panel B reflect the most likely scenarios according to available trials1-3: a relative risk reduction of 20% and prevention of 1 breast-cancer death. The data for Switzerland, reported in the same study, show similarly overly optimistic expectations. How can women make an informed decision if they overestimate the benefit of mammography so grossly?
The Swiss Medical Board’s report was made public on February 2, 2014 (www.medical-board.ch). It acknowledged that systematic mammography screening might prevent about one death attributed to breast cancer for every 1000 women screened, even though there was no evidence to suggest that overall mortality was affected. At the same time, it emphasized the harm — in particular, false positive test results and the risk of overdiagnosis. For every breast-cancer death prevented in U.S. women over a 10-year course of annual screening beginning at 50 years of age, 490 to 670 women are likely to have a false positive mammogram with repeat examination; 70 to 100, an unnecessary biopsy; and 3 to 14, an overdiagnosed breast cancer that would never have become clinically apparent.5 The board therefore recommended that no new systematic mammography screening programs be introduced and that a time limit be placed on existing programs. In addition, it stipulated that the quality of all forms of mammography screening should be evaluated and that clear and balanced information should be provided to women regarding the benefits and harms of screening.
The report caused an uproar and was emphatically rejected by a number of Swiss cancer experts and organizations, some of which called the conclusions “unethical.” One of the main arguments used against it was that it contradicted the global consensus of leading experts in the field — a criticism that made us appreciate our unprejudiced perspective resulting from our lack of exposure to past consensus-building efforts by specialists in breast-cancer screening. Another argument was that the report unsettled women, but we wonder how to avoid unsettling women, given the available evidence.
The Swiss Medical Board is nongovernmental, and its recommendations are not legally binding. Therefore, it is unclear whether the report will have any effect on the policies in our country. Although Switzerland is a small country, there are notable differences among regions, with the French- and Italian-speaking cantons being much more in favor of screening programs than the German-speaking cantons — a finding suggesting that cultural factors need to be taken into account. Eleven of the 26 Swiss cantons have systematic mammography screening programs for women 50 years of age or older; two of these programs were introduced only last year. One German-speaking canton, Uri, is reconsidering its decision to start a mammography screening program in light of the board’s recommendations. Participation in existing programs ranges from 30 to 60% — variation that can be partially explained by the coexistence of opportunistic screening offered by physicians in private practice. At least three quarters of all Swiss women 50 years of age or older have had a mammogram at least once in their life. Health insurers are required to cover mammography as part of systematic screening programs or within the framework of diagnostic workups of potential breast disease.
It is easy to promote mammography screening if the majority of women believe that it prevents or reduces the risk of getting breast cancer and saves many lives through early detection of aggressive tumors.4 We would be in favor of mammography screening if these beliefs were valid. Unfortunately, they are not, and we believe that women need to be told so. From an ethical perspective, a public health program that does not clearly produce more benefits than harms is hard to justify. Providing clear, unbiased information, promoting appropriate care, and preventing overdiagnosis and overtreatment would be a better choice.
The views expressed in this article are those of the authors and do not necessarily reflect those of all members of the expert panel of the Swiss Medical Board.
Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
This article was published on April 16, 2014, at NEJM.org.
From the Institute of Biomedical Ethics, University of Zurich, Zurich (N.B.-A.), and the Institute of Social and Preventive Medicine and Clinical Trials Unit Bern, Department of Clinical Research, University of Bern, Bern (P.J.) — both in Switzerland; and the Division of Medical Ethics, Department of Global Health and Social Medicine, Harvard Medical School, Boston (N.B.-A.). Dr. Biller-Andorno is a member of the expert panel of the Swiss Medical Board; Dr. Jüni was a member of the panel until August 30, 2013.
http://www.bloomberg.com/dataview/2014-04-17/how-americans-die.html?alcmpid=view
Particularly interesting observations on Alzheimer’s spending: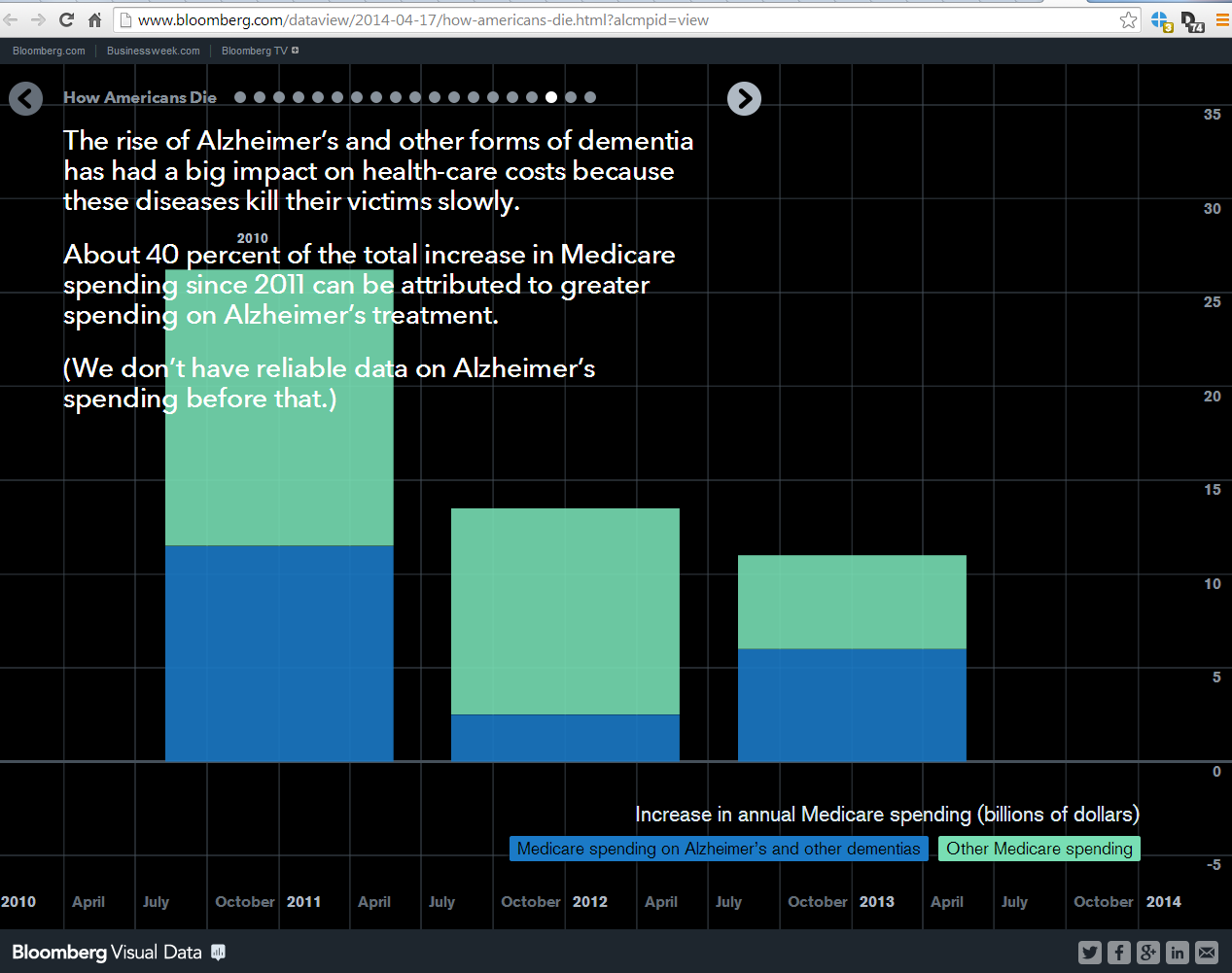
http://www.nuviun.com/nuviun-digital-health
good infographics…
http://storyofdigitalhealth.com/infographic/
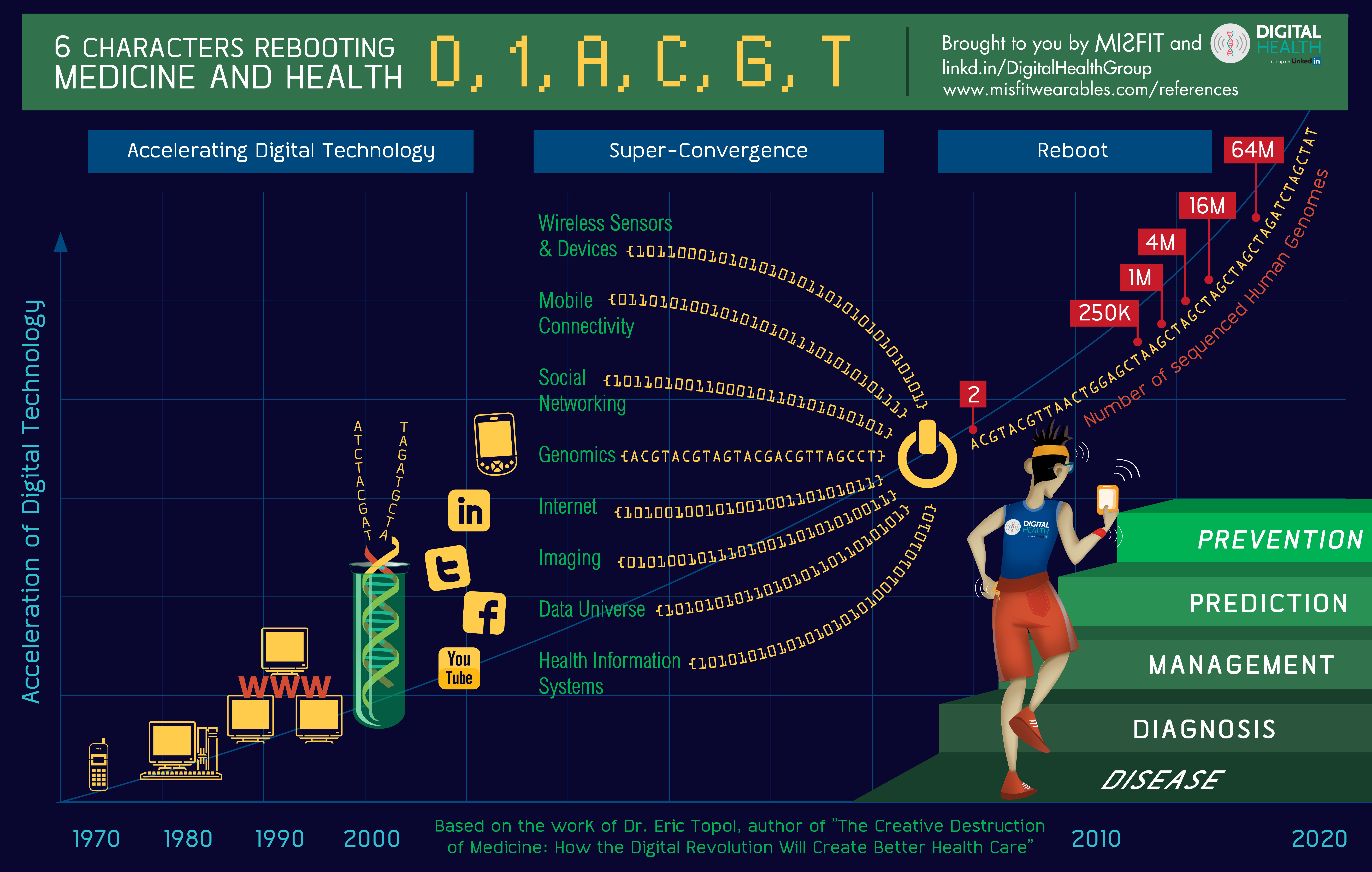
Infographic
I created this conceptual infographic illustrating the increasing health benefits achievable with digital health with the great team at Misfit Wearables. You can download a high-resolution version by clicking on the image.
References:
Number of people sequenced
“250,000 human genomes will be fully sequenced by the end of 2012, 1 million by 2013, and 5 million by 2014″ -Topol, Eric (2011-12-02). The Creative Destruction of Medicine: How the Digital Revolution Will Create Better Health Care (p. 102). Perseus Books Group. Kindle Edition.
Also, compliments of Story of Digital Health strategic partner nuviun, there’s this interactive diagram of the digital health landscape…
PCMHs and ACOs are complementary approaches to improving care delivery. Medical homes require strong links to specialists and hospitals, while ACOs—which are accountable for the full continuum of health services—require a strong grounding in primary care. The authors suggest the following payment approaches to promote integration of PCMHs and ACOs:
http://www.commonwealthfund.org/Publications/In-Brief/2014/Apr/Structuring-Payment-to-Medical-Homes.aspx?omnicid=20
April 7, 2014
Authors: Samuel T. Edwards, Melinda K. Abrams, Richard J. Baron, Robert A. Berenson, Eugene C. Rich, Gary E. Rosenthal, Meredith B. Rosenthal, and Bruce E. Landon
Journal: Journal of General Internal Medicine, published online April 1, 2014
Contact: Bruce E. Landon, M.D., M.B.A., Harvard Medical School, landon@hcp.med.harvard.edu
Summary Writers: Martha Hostetter
Access to full article: View Article
The patient-centered medical home (PCMH) model aims to transform primary care practice through the use of multidisciplinary teams and a shift from “reactive visit-based care to proactive population health management.” Currently, medical home providers are reimbursed with a blend of fee-for-service payments and additional compensation for services provided outside of office visits, including care coordination. Writing in the Journal of General Internal Medicine, Harvard Medical School’s Samuel T. Edwards, M.D., and colleagues consider how the PCMH payment model could evolve to keep pace with health care payment reforms launched by the Affordable Care Act, most notably the “shared savings” approach used by many accountable care organizations (ACOs).
PCMHs and ACOs are complementary approaches to improving care delivery. Medical homes require strong links to specialists and hospitals, while ACOs—which are accountable for the full continuum of health services—require a strong grounding in primary care. The authors suggest the following payment approaches to promote integration of PCMHs and ACOs:
As a promising model of care delivery, the PCMH “can serve as a lynchpin of ACOs,” the authors say. For their part, ACOs will need to support this model within their organizations.
S. T. Edwards, M. K. Abrams, R. J. Baron et al., “Structuring Payment to Medical Homes After the Affordable Care Act,” Journal of General Internal Medicine, published online April 1, 2014.
PDF: 1742_Herrin_community_factors_hosp_readmission_rates_HSR_04_09_2014_itl
Community Factors and Hospital Readmission Rates
April 16, 2014
Authors: Jeph Herrin, Justin St. Andre, Kevin Kenward, Maulik S. Joshi, Anne-Marie J. Audet, and Stephen C. Hines
Journal: Health Services Research, published online April 9, 2014
Contact: Jeph Herrin, Ph.D., Division of Cardiology, Yale University School of Medicine, jeph.herrin@yale.edu
Summary Writers: Deborah Lorber
Access to full article: View Article
A majority of the variation seen in U.S. hospitals’ readmission rates for heart attack, heart failure, and pneumonia can be attributed to hospitals’ location, rather than to the quality of care provided in individual hospitals. Community factors most strongly associated with lower hospital readmission rates include more general practitioners and fewer specialists per capita and the presence of high-quality nursing home care.
Readmission to the hospital shortly after discharge has been recognized as an indicator of poor health system coordination. Since 2009, the Centers for Medicare and Medicaid Services has been publicly reporting 30-day readmission rates for heart attack, heart failure, and pneumonia. And in 2013, Medicare began linking payments to hospitals to how well they perform on these measures, leading hospitals to focus on improving their rates. Previous studies have looked for relationships between readmission rates and hospital characteristics, like size or teaching status, or patient-level factors, like race or health literacy. This article, supported by The Commonwealth Fund, looks at the association between readmission rates and local community characteristics.
If community factors explain a substantial amount of the variation in hospital readmission rates, then programs that penalize hospitals with readmission rates above a certain threshold may not be appropriate, the authors say. Other initiatives might be more effective, such as the Affordable Care Act’s Community-Based Care Transitions Program, which allows community-based organizations to receive a bundled payment that covers the costs of services needed to help patients transition from hospital to home.
The authors examined all hospitals with publicly reported 30-day readmission rates for patients with acute myocardial infarction, heart failure, or pneumonia who were discharged between July 1, 2007, and June 30, 2010. Readmissions data were then linked with publicly available county data from the Area Resource File, the U.S. Census, Nursing Home Compare, and the Neilsen PopFacts data set. The final sample included 4,073 hospitals.
Population characteristics at the county level explain a large portion of the variation in hospital readmission rates for certain major medical conditions. Instead of strictly penalizing hospitals for exceeding certain thresholds, policymakers should focus on programs that help patients transition from hospital to home.
J. Herrin, J. St. Andre, K. Kenward et al., “Community Factors and Hospital Readmission Rates,” Health Services Research, published online April 9, 2014.
“Whenever you put information out there, creativity and innovation flourish,” she said. “This is going to be such a giant leap forward in terms of what we’re doing in health care today, what works, what doesn’t work and what it should cost.” But for that to happen “there needs to be some “pretty powerful computing and some savvy tech gurus to help slice and dice this information in meaningful ways for consumers”
New York is sponsoring a contest — the Health Innovation Challenge — that asks the tech-savvy, including coders and developers, to put health data to use keeping costs down, increasing quality and improving efficiency. Winners receive cash, and their ideas will be put to work in the state government.
Shah said releasing the data — and allowing researchers, entrepreneurs and consumers to dig into it — could “democratize” health care in a way that has already happened with the way people buy cars or plane tickets: It will allow them to compare cost and quality.
Instead of making decisions based on quality, people tend to pick their providers based on where their doctor recommends they should go, and that might mean where she did her residency or a specialist whom she plays golf with, he said. New data may allow people to comparison shop for medical care.
While Shah acknowledged a “special” relationship between a patient and a doctor that includes treatment plans and communication in ways that won’t be picked up in data, a colonoscopy should be the same everywhere.
Rather than taking doctors’ recommendations, entrepreneurs will take data, repackage it and show people which hospitals have the longest average stays, which charge the most for a procedure, and which have the highest infection rates.
“Often, we find that high quality equals lower costs,” he said. That’s because the most cost-effective procedures tend to be the ones where patients receive proper medications, do not have to be treated for hospital-based infections, and where providers work as a team to make sure quality measures are met.
As more people — or their employers — choose low-premium, high-deductible plans, the cost of a knee surgery or an imaging scan becomes more important to the consumer than when insurance covered everything.
http://www.usatoday.com/story/news/nation/2014/04/16/new-cms-data-inspires-entrepreneurs/7735469/
WASHINGTON — As the government moves toward more medical “transparency” by releasing a slew of new data— including Medicare provider payment data last week — entrepreneurs are creating new products to help consumers use the data to choose quality, lower-cost care.
Beyond the profit motive, some entrepreneurs hope to use the data to keep costs down on new medical products they create, help the government suss out fraud or unusual activity, and to persuade doctors to use the best practices gathered from their peers — something that was difficult to do when pricing information was not available.
CHART: See how much Medicare paid each doctor in U.S.
“I think this data transparency is one of the major keys to transformation of the entire health care system,” said Robert Grajewski, president of Edison Nation Medical, a group that works to remove barriers for getting medical devices to the market. “In health care, it’s very confusing to know what the pricing is, not just for the device, but for the overall procedure. This helps us have a benchmark that needs to be achieved or overcome to improve care and overcome costs.”
The provider payment data released by the Centers for Medicare & Medicaid Services has Grajewski looking at why prices are higher for one doctor over another, why a doctor might choose a brand name over a generic medication, and why a doctor might choose surgery over physical therapy. The data became available after a court order lifted an injunction sought by the American Medical Association had been in place since 1979.
Grajewski isn’t the only one. Mercom Capital Group released a report Monday that found venture capital funding for health care information technology hit $858 million in the first quarter of this year. That includes $398 million in 103 new deals for consumer-focused technology, such as mobile apps.
“We’ve been tracking these numbers since 2010, and this quarter was the biggest number ever,” said Raj Prabhu, Mercom’s CEO. “$858 million is a huge number — in 2010, I don’t think we saw $200 million.”
Much of the momentum is coming from inventors who hope to create shopping applications that allow consumers to compare prices and outcomes on their smart devices. These include apps such as GoodRX, which allows consumers to compare medication prices at different pharmacies; NerdWallet Health, which allows people to compare hospital prices by locations; and an app from Consumer Reports that lets people compare prices for hip and knee replacements.
“Ever since the government started releasing data, this has been great for these kinds of companies to turn into useful applications,” Prabhu said.
“Every person is a health care consumer,” he said. “It’s so massive — nobody wants to miss the boat.”
Ceci Connolly, managing director of PWC’s Health Research Institute, said she expects the data to ultimately help the health care industry itself.
“Whenever you put information out there, creativity and innovation flourish,” she said. “This is going to be such a giant leap forward in terms of what we’re doing in health care today, what works, what doesn’t work and what it should cost.”
But for that to happen, there needs to be some “pretty powerful computing and some savvy tech gurus to help slice and dice this information in meaningful ways for consumers,” she said. Someone could use the CMS data to look at trends in hip surgeries: Is it much higher for one hospital than at others? A consumer might reconsider whether he actually needs surgery from a particular doctor. Or are there relatively few hip surgeries at the local hospital? The consumer might consider going to a doctor who performs a lot of hip surgeries.
Someone else might take the CMS data and compare it to CMS’s Five-Star Quality Rating System data, Connolly said.
“The whole promise of big data is not just any one data set, but it’s the way you can bring them together and analyze them across many,” she said.
New York is sponsoring a contest — the Health Innovation Challenge — that asks the tech-savvy, including coders and developers, to put health data to use keeping costs down, increasing quality and improving efficiency. Winners receive cash, and their ideas will be put to work in the state government.
It comes after the launch of the state’s transparency project, Open.NY.gov, which features data that state agencies have been ordered to catalog for the public.
“For a long time, the medical establishment has talked about patient-centered care,” New York State Department of Health Commissioner Nirav R. Shah. “But largely, it’s still been about hospital-centered care, doctor-centered care.”
Shah said releasing the data — and allowing researchers, entrepreneurs and consumers to dig into it — could “democratize” health care in a way that has already happened with the way people buy cars or plane tickets: It will allow them to compare cost and quality.
Instead of making decisions based on quality, people tend to pick their providers based on where their doctor recommends they should go, and that might mean where she did her residency or a specialist whom she plays golf with, he said. New data may allow people to comparison shop for medical care.
While Shah acknowledged a “special” relationship between a patient and a doctor that includes treatment plans and communication in ways that won’t be picked up in data, a colonoscopy should be the same everywhere.
Rather than taking doctors’ recommendations, entrepreneurs will take data, repackage it and show people which hospitals have the longest average stays, which charge the most for a procedure, and which have the highest infection rates.
“Often, we find that high quality equals lower costs,” he said. That’s because the most cost-effective procedures tend to be the ones where patients receive proper medications, do not have to be treated for hospital-based infections, and where providers work as a team to make sure quality measures are met.
As more people — or their employers — choose low-premium, high-deductible plans, the cost of a knee surgery or an imaging scan becomes more important to the consumer than when insurance covered everything.
http://www.washingtonpost.com/national/health-science/scientists-embark-on-unprecedented-effort-to-connect-millions-of-patient-medical-records/2014/04/15/ea7c966a-b12e-11e3-9627-c65021d6d572_story.html
The data — from every patient treated at one of New York’s major hospital centers over the past few years — include some of the most intimate details of a life. Vital signs. Diagnoses and conditions. Results of blood tests, X-rays, MRI scans. Surgeries. Insurance claims. And in some cases, links to genetic samples.
Nothing of this scale has been built before, and researchers say the potential of the network to speed up research efforts and to answer questions that have long vexed scientists cannot be overstated. But the creation of the network presents tricky ethical questions about who owns and controls the data, how to protect patient privacy and how research questions will be prioritized.
“Both the opportunity and the anxiety are pretty electrifying,” Francis S. Collins, director of the National Institutes of Health, said in an interview.
The origins of the patient project lie in an obscure part of the 2010 Affordable Care Act. As part of the nation’s health-care overhaul, Congress created an independent nonprofit group to help patients and their doctors make better-informed decisions about care. Dubbed the Patient-Centered Outcomes Research Institute, or PCORI, and based in the District, the organization’s mandate is to launch, fund and coordinate research on “comparative effectiveness” — to find out which drugs, devices and treatment options are more effective than others.
Do certain sets of behavioral interventions work better than others for weight control, for example? Might certain antibiotics work better for cystic fibrosis patients, based on their genetic profile?
Such questions have been surprisingly difficult to answer, despite the thousands of clinical trials published every year.
Physicians have long grumbled that few studies can be translated into practical advice. Some studies are too small to draw any definitive conclusions. Others include patients diagnosed with a single condition, while most patients are more complicated — they suffer from multiple issues. It isn’t uncommon for studies to contradict each other, and there’s no way for clinicians to know which one is right, because they often use different methodologies.
“The whole idea was to create a way to do the kind of research that would inform the real world,” explained Eugene Rich, who researches health-care effectiveness for Mathematica Policy Research, based in Princeton, N.J.
The database — an idea that has been talked about for years by everyone from insurance companies to Google but has never been successfully executed — holds the hope that some of those obstacles can be overcome.
“We will be able to get answers with a degree of certainty that we’ve never had before,” said Joe V. Selby, PCORI’s executive director, who calls the patient records network “the holy grail” of health-care research.
Collins said the value of the network is that it gives scientists the ability to ask an endless number of questions about a massive patient population with great speed and little cost.
In the randomized trials that NIH typically supports, “you have to enroll patients from the very beginning, and that’s a big infrastructure-building process that can take quite some time. And once a trial has been conducted, the whole thing has to be taken down again,” Collins said.
“It’s a great way to answer one specific question, but it’s not an efficient way to ask lots of questions,” he explained.
Before PCORI’s vision can be realized, the project’s leaders must overcome numerous hurdles.
The technical challenges of the project are enormous. The specter of the botched launch of HealthCare.gov haunts anyone trying to get large numbers of separate computer systems to talk to each other. But it is the larger questions about governance that have triggered conflict and worry in the nation’s health-care community.
How will research questions be prioritized? How should disagreements be resolved?
Should pharmaceutical companies and insurers be able to access the records and, if so, under what circumstances? What about the Centers for Disease Control and Prevention? The information could help epidemiologists track outbreaks and clusters of disease in a way they have never done before.
And, critically important to the multibillion-dollar pharmaceutical industry, how will the Food and Drug Administration view this type of research when considering applications for new drugs or in recalling old ones?
PCORI was never imagined to be the custodian of this kind of data network. It was designed to launch and fund research in a manner similar to NIH and the National Science Foundation. But it did not get nearly the same kind of funding.
President Obama’s budget request for fiscal 2015 included $30.4 billion for NIH and nearly $7.3 billion for NSF. But PCORI, which is funded through several streams, gets only about $500 million annually. Large, randomized clinical trials such as the ones NIH does for important questions cost upwards of $150 million, meaning that PCORI has enough to fund only two or three a year.
“So about a year ago, PCORI started talking about whether there is another model that is different from the NIH model, which would be more about embedding clinical studies in the fabric of day-to-day care,” said Robert W. Dubois, chief science officer for the National Pharmaceutical Council, a health policy research group funded by the industry.
The PCORI network, which is being built at a cost of nearly $100 million, would also be a way to pinpoint patients with certain criteria who could be invited to join a clinical trial. As it stands today, identifying patients eligible for trials is often time-consuming, expensive and hit-or-miss. Researchers must use a variety of tools to get enough participants, including reaching out to a network of doctors who then contact their patients and the old-fashioned method of putting up fliers in places where people with the criteria they are looking for congregate.
The new national patient network will comprise 11 sub-networks that include records from New York and Chicago, children’s hospitals, Kaiser Permanente and other groups. Each participating organization retains all the personally identifiable data and would have the right to accept or decline a research proposal. If a research project is greenlighted, each of the smaller networks would analyze its own databases and return an anonymized, aggregated response to the researcher.
“The raw data is not what is being shared. That remains with the institution that the patient trusts,” said Devon McGraw, director of the health privacy project for the Center for Democracy and Technology and head of the data privacy task force for PCORI.
Privacy experts say the general consent forms that patients sign when they get treatment should allow the use of data already collected in the aggregate. Hospitals and other organizations participating in the project don’t have any plans to explicitly inform patients about this. If researchers wanted doctors to collect additional data as part of a clinical trial, the researchers would clearly have to get a patient’s consent. But what about projects that involve more detailed analysis of individual patient histories?
One aspect of the project that was highlighted by researchers involved is that it has included patients at every step. Patient panels have been convened to help suggest research questions, and patients serve on the committees looking at privacy and data security.
“As a provider, I may be interested in how a serum marker changes with a treatment. But patients may be more interested in how it affects how they feel, their ability to exercise and eat,” she said.
Brian Currie, vice president for medical research for the Montefiore Medical Center, the university hospital for the Albert Einstein College of Medicine in the Bronx, which is participating in the New York network, said the number of questions are understandable given the historical barriers between different types of institutions that have prevented this research in the past.
“It’s pushing all the fronts on how medical institutions do research,” Currie said.